We've come to the time of year when allergies and respiratory viruses like the common cold become more prevalent, and I am spending a good amount of time with my friends, family, and patients discussing how to tell the difference between the symptoms of these typical yearly bringers of snot and sniffles (irritating but generally benign) and those of Covid-19, the clinical scenario caused by the novel coronavirus.
First and foremost, I believe we cannot tell the difference with 100 percent confidence. The novel coronavirus causing Covid-19 simply has the ability to affect too many body systems and can therefore lead to such a wide variety of symptoms that we will never be able to give a perfect answer to this question. Just take a look at the list of symptoms on the C.D.C.'s website that could be due to Covid-19 -- from fever, cough, and chills to gastrointestinal upset or runny nose -- and you can easily see the problem.
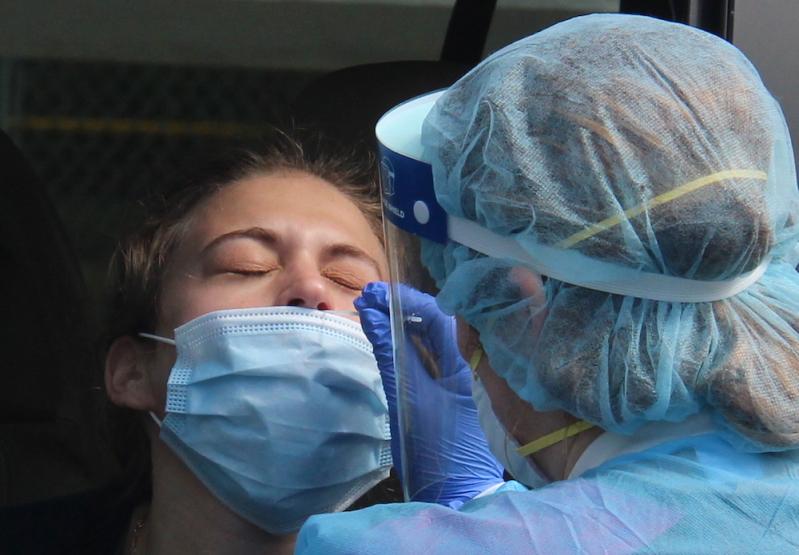
The only way to come closer to knowing whether you have Covid-19 is to get tested, and even that can be inaccurate, depending on the timing and type of the test. If you are exposed to the novel coronavirus and get tested in the, say, two to three days immediately after exposure, it is possible you won't have built up enough of a viral load in your nasopharyngeal airway yet to lead to a positive test. Or, let's say you wait five or six days to get tested after exposure, (we hope) staying in isolation up to that point, but then get a rapid antigen test instead of what's known as a P.C.R. test, the latter of which may take longer but is more reliable.
Despite these pitfalls and flaws, testing combined with our common sense remains the best approach we have to containing Covid-19, but it is important to recognize that there are many variables across the board that complicate giving good recommendations.
If you're a parent who recently had your kid restart school and you're frustrated by the many, many symptoms that can get your child sent home right now, or if you're an employee who was sent home from work because of a mild cough and want to know why, I want to spend some time explaining, from the medical side of the fence, what is making all of this so difficult to navigate.
For example, if you or your child is experiencing a runny nose, itchy eyes, maybe some postnasal drip with an associated mild cough, and you get these symptoms every time the pollen count is up or your cat sleeps on your pillow, and you don't have a fever or any close contacts who have tested positive for Covid-19, then I do think it is likely you have allergies. You might try your usual allergy regimen, say a non-sedating antihistamine like Claritin or Zyrtec, or maybe take the prescription medicine your primary doctor or allergist gives you, and if it is allergies, I would expect the symptoms to get better.
But the only way to know would be to get tested because there are patients with Covid-19 who exhibit only relatively mild upper respiratory symptoms.
Now, let's take a slightly different spin. Say you have a runny nose, mild sore throat, stuffy ears, maybe a mild cough, and feel run down. Most years, particularly in the absence of a fever or any really severe symptoms, I'd say with high confidence that you have a cold, and recommend rest, fluids, etc., mainly if you haven't lost your sense of smell or sense of taste, as especially these last two appear to be more common in patients with Covid-19.
But I will not be able to say that it's just a cold and not Covid-19 without testing, and even then, just in case your test results in a false negative, I will still probably recommend staying home (if you can) until you are 10 days past the onset of symptoms.
Because we just don't know for certain.
I know this uncertainty, like so many aspects of 2020, is a huge cause of stress and anxiety and frustration. I know that access to testing has been sporadic in many places, and I'm grateful for the efforts that my employer Stony Brook Southampton Hospital has made to make it more available locally, information concerning which can be found on the hospital's website.
Ultimately, as much as I would like to do so, I can't take away the uncertainty, but it is to be hoped that by explaining a little more of the medical point of view that's driving some of these policies, I can alleviate a little of the frustration.
--
Joshua Potter, D.O., is a physician with Stony Brook Southampton Hospital's Meeting House Lane Medical Practice who specializes in family and neuromusculoskeletal medicine. He oversees the practice's Shelter Island office. Opinions expressed in this column are his personal and professional views and not necessarily those of his employer.